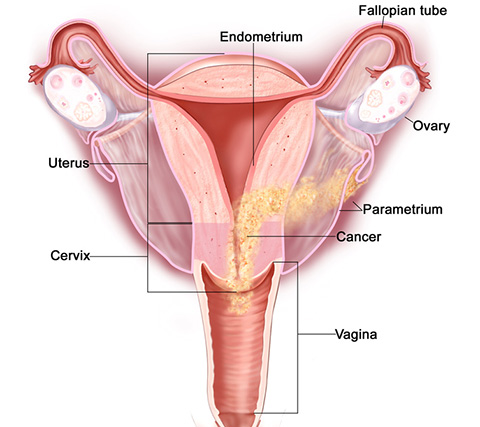
 The lower part of the uterus (womb) is the cervix. The uterus has two parts. The upper part, called the body of the uterus, is where a fetus grows. The body of the uterus connected to the vagina, or birth canal through the cervix, in the lower part.
The lower part of the uterus (womb) is the cervix. The uterus has two parts. The upper part, called the body of the uterus, is where a fetus grows. The body of the uterus connected to the vagina, or birth canal through the cervix, in the lower part.
Cancer of the cervix (also called cervical cancer) begins in the cells lining the cervix. These cells do not suddenly change into cancer. At first, the normal cells of the cervix gradually change into pre-cancer cells and then, later on, turn into cancer. These changes perhaps called dysplasia. The change can take many years but sometimes happen faster. The Pap test can find these changes and treated to prevent cancer.
There are two main types of cancer of the cervix. About 8 to 9 out of 10 are squamous cell carcinomas. This type of cancer is made up of cells that are like squamous cells that cover the surface of the cervix.
Rest are adenocarcinomas. These kinds of cancers begin in the gland cells that form mucus. Less often, cancer has features of both types and thus called adenosquamous or mixed carcinoma.
Some distinct types of cancer also can arise in the cervix. These other types (such as melanoma, sarcoma, and lymphoma) happen most often in other parts of the body. If you think you have cervical cancer, you better consult your doctor and ask him to justify your cancer type.
This information is only of the more common types of cervical cancer, not the rare ones.
How many women get cancer of the cervix?
The American Cancer Society’s estimates for cancer of the cervix in the United States for 2015 are:
- About 12,900 new cases of invasive cervical cancer (cancer that has spread beyond the cervix)
- About 4,100 deaths from cervical cancer
Cervical pre-cancers are much more common than invasive types of cancer.
Most cases of cervical cancer seen in women younger than 50. Women over 50, however, still get cervical cancer.
The death rate from cervical cancer has gone down a lot over the last 30 years. The main reason for this change is the use of screening to find cervical cancer early.
Signs and symptoms of cervical cancer
Most often early cervical pre-cancers or cancers have no signs or symptoms. That is why it is important for women to have regular screening for a Pap test (which may be combined with a test for HPV). Symptoms often do not start until cancer has further spread to nearby areas. You should report any of the followings to your doctor right away:
- Irregular vaginal bleeding, such as bleeding after menopause, bleeding after sex, spotting and bleeding between periods, or having periods that are heavier or longer than normal. Bleeding after douching or after a pelvic exam may also occur.
- An unexpected discharge from the vagina (not your normal period)
- Pain during sex
Of course, these symptoms do not mean that you have cancer. They can also be caused by something else. But you must check with a doctor to find out.
Survival rates for cancer of the cervix
Some people with cancer may want to know the survival rates for their type of cancer.
The 5-year survival rate refers to the percent of patients who live at least five years after finding that they have cancer. Many of these patients live much longer than five years. Also, these rates look at deaths from any cause. People with cancer may die from things other than cancer, and these rates do not take that into account.
To acquire 5-year survival rates, doctors have to look at people who were treated at least 5 years ago. Better treatments since then may mean a better outlook for people now found to have cervical cancer.
The numbers below come from the National Cancer Data Base as published in the 7th edition of the AJCC Cancer Staging Manual, and are based on people diagnosed between 2000 and 2002.
Stage 5-Year Observed Survival Rate
0 93%
IA 93%
IB 80%
About treatment
The treatment options for cervical cancer depend mostly on the stage of cancer. Once your cancer is staged, after that your doctor will tell you about what choices you have. If there is anything you do not understand, ask for it to be explained. Factors other than the stage of cancer that might have an impact on your treatment decision include your age, your overall health, and your preferences.
Common treatments for cervical cancer include
- Surgery
- Radiation therapy
- Chemotherapy
- Targeted therapy
A few primary cervical cancers are only treated with surgery alone. Most cervical cancers are also treated with radiation combined with chemotherapy.
Surgery for cancer of the cervix
Surgery is generally used to treat initial cancers of the cervix.
Cryosurgery
A metal probe cooled with liquid nitrogen is put in the vagina and on the cervix. It kills the abnormal cells by freezing them. Cryosurgery used for the treatment of 0 stage cancers (carcinoma in situ), but not used for treating invasive cancer.
Laser surgery
A laser beam is used to burn off cells or to remove a small piece of tissue for study. Laser surgery is used for 0 stage cancers (carcinoma in situ), but not for invasive cancer.
Conization
A cone-shaped piece of tissue is removed from the cervix. It is done using a surgical or laser knife (cold knife cone biopsy) or using a thin wire heated by electricity (sometimes called a LEEP or LEETZ procedure). This approach can be used to find or to treat very early stage (0 or I) cancer.
Hysterectomy
The cervix and uterus are removed in a hysterectomy and this is known as a simple hysterectomy. The ovaries and fallopian tubes or pelvic lymph nodes may be taken out during the same operation, but this is not a part of every hysterectomy.
Sometimes also called a total hysterectomy. The uterus is taken out either through a cut (incision) in the front of the belly (abdomen) or through the vagina. Laparoscopy used with either of these methods. A long, thin tube called laparoscope with a small camera on end put into the belly through small cuts in the skin. This helps the surgeon see inside and use small tools to remove organs. Because the cuts are small, the patient may recover faster.
Some very early stage cervical cancers usually treated with a hysterectomy. A hysterectomy also used for some stage 0 cancers if the cone biopsy did not remove all cancer.
Radical hysterectomy
For this operation, the surgeon removes more than just the uterus. They removed the tissues next to the uterus and the upper part of the vagina next to the cervix. This surgery, along with a pelvic lymph node dissection is the usual treatment for stages I and, less often, some stage II cervical cancers, especially in young women.





